

Last Sunday I talked with a woman who said, “COVID is making me so OCD!” She’s been working from home for months, in a state that is tightly locked down. With her normal summer activities disrupted, her isolation has been filled with painting the baseboards and other wood trim, hanging her growing son’s clothes hooks higher, and weeding flowerbeds for hours.
“I get down on the floor to exercise and all I can focus on is the pulled place in the rug. And then I look out the window and feel like I ought to be out there raking leaves, even though they’re only half down. And this morning, I rearranged books size and color as well as type.
“See? Completely OCD.”
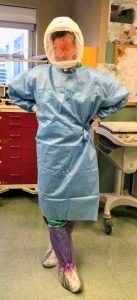
OCD (obsessive-compulsive disorder) is a label that’s tossed around loosely, like beautiful or crazy. The woman I talked to is a good example. OCD is casually applied to people who are finicky or particular about some one thing (e.g., straightening picture frames) rather than people with serious mental health problems that interfere with living a healthy, comfortable life.
Technically, OCD applies only to people who use obsessive thoughts and/or compulsive behaviors in an attempt to deal with anxiety and fear. It’s a coping mechanism—another way to get through the day.
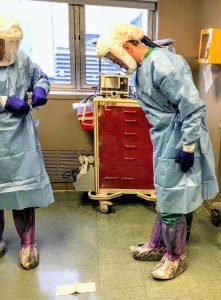
Today, OCD is viewed by researchers as a spectrum, much like autism. It often develops in people with a genetic predisposition to anxiety disorders and mental illness, and this is the group most likely to develop true OCD in response to COVID. For these people, when the threat diminishes, the attempts to reduce the threat do not go away—and may worsen.

Ideally, people with OCD receive treatment (usually a combination of medication and behavioral or exposure therapy) to deal with the condition. One of the major goals of treatment is learning not to try to avoid their fears. Instead, patients with OCD work to balance exposure to triggering conversation and information with healthful activities such as exercise, spending time outside, developing good sleep habits, etc., while doing things in line with personal and work-related goals.

The spread of COVID has caused a spike in anxiety and fear for everyone (with the possible exception of some diehard deniers). The constant need for vigilance has forced nearly everyone to change daily habits, focus on ways to stay safe and well, and then to act on them. People who compulsively watch the news or spend hours on social media typically are more fearful.

Many people previously diagnosed with OCD are suffering greatly. Medical experts’ advice to wear a mask, wash hands thoroughly and often, avoid touching their faces, avoid being around sick people, disinfect surfaces most often touched, and socially distance requires a lot of attention throughout the day. People with a germ phobia may be unable to attend to anything else!
Ideally, the OCD sufferer will do but not overdo: for example, to wash hands for twenty seconds and no longer—to focus on having done the hand washing, not on feeling clean. Tip: if you wonder whether you are over-doing it, you probably are.
A germ phobia as related to OCD is obvious. But according to Dr. Rachel Ginsberg of Columbia University, there are several possible impacts of the pandemic on OCD patients.
“Other types of OCD that can be triggered by this pandemic include somatic obsessions (concerns with illness or disease, such as headaches), sensory-focused symptoms (obsessing over sensations in the body or perceived feelings on the skin’s surface), feelings of over responsibility and inappropriate guilt (e.g. related to spreading the illness), and harm OCD (e.g. fear that one will be responsible for something terrible happening, such as unknowingly causing others’ death).
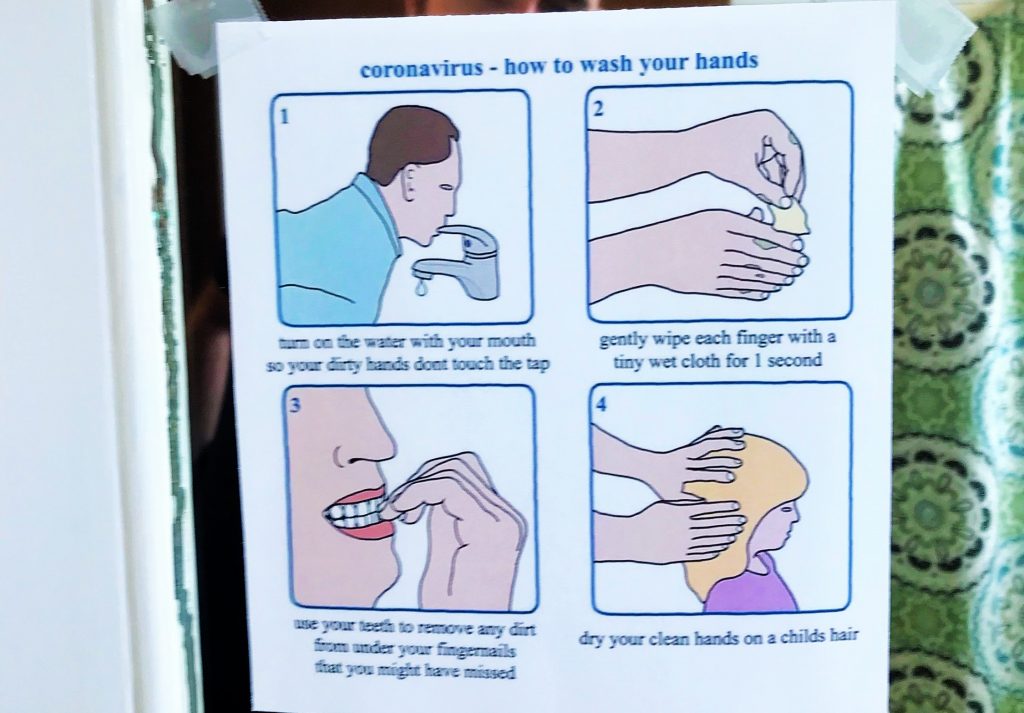
Additional OCD symptoms might include magical thinking, superstitious fears, fear of harm coming to self or others because of not being careful enough (fear of spreading germs if you were unknowingly COVID-positive or asymptomatic), and religious obsessions or excessive fear of right vs. wrong.

Moreover, OCD symptoms may include needing to know or remember information related to updated guidelines, and related excessive information gathering and checking. In addition to handwashing and cleaning, compulsions that might present or worsen could include mental reviewing (of where you have been, how far you stood from someone else, what you might have touched), needing to tell/ask/confess to others, superstitious behaviors, and health-related compulsions (e.g. asking for excessive reassurance from doctors about health symptoms).”
Dr. Rachel Ginsberg

For some people, the pandemic is just proof that they were right all along: the world is truly a dangerous place. For mentally healthy people, this danger will pass when the pandemic passes: they are highly unlikely to develop lifelong OCD. In non-OCD people, when the threat diminishes, the compulsive threat-based behaviors will diminish.
Bottom Line: People are different. (You heard it here first!) In this instance, people will vary widely in the extent, severity, and duration of COVID-triggered obsessions and compulsions.

